7 Steps to Weight Loss in Type 2 Diabetes


Table of Contents
- The Physiology: Weight, Insulin, and Glucose
- Step 1: Set Short-Term and Long-Term Goals
- Step 2: Master Portion Sizes
- Strategies:
- Step 3: Implement Dietary Changes
- Increase Fruits and Vegetables
- Reduce Added Sugar and Processed Foods
- Step 4: Incorporate Regular Physical Activity
- Step 5: Aim for 150 Minutes of Exercise Weekly
- Step 6: Monitor and Adjust
- Step 7: Maintain Commitment and Resilience
- The Clinical Connection: Weight Loss and Glycemic Control
- Conclusion
- Frequently Asked Questions
- Why is it harder to lose weight with Type 2 diabetes?
- What is the Plate Method for diabetic weight loss?
- Can I stop my medication if I lose significant weight?
- How does exercise specifically help with weight loss in diabetics?
Type 2 diabetes is a prevalent chronic condition that, if poorly managed, can drastically impact quality of life. However, with adequate knowledge, lifestyle modifications, and medical intervention, these risks can be mitigated.
Weight management is a critical component of this care plan. Obesity and being overweight elevate the risk of developing the disease and worsen health complications for individuals already diagnosed. The first step toward effective management is understanding the physiological relationship between weight and blood glucose.
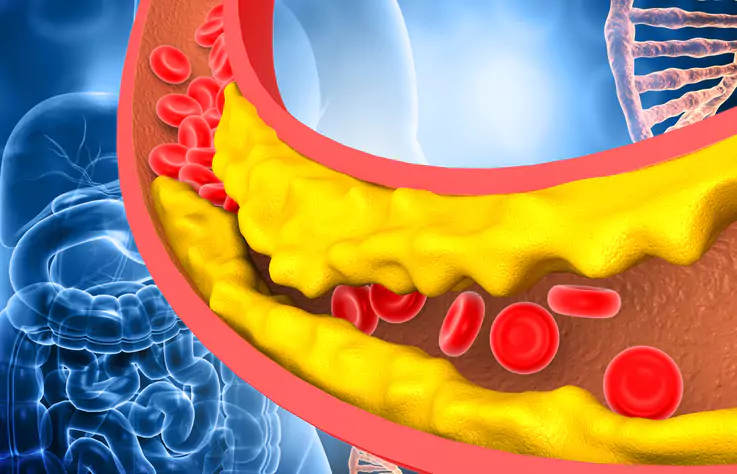
The Physiology: Weight, Insulin, and Glucose
Insulin is the hormone that regulates blood glucose levels. In a healthy system, it allows glucose to enter cells for energy. In Type 2 diabetes, the body develops insulin resistance, meaning cells respond less effectively to insulin. This leads to hyperglycemia (high blood sugar).
Excess weight, especially abdominal fat, worsens insulin resistance by releasing chemicals that disrupt metabolic and cardiovascular systems. This creates a cycle:
- Insulin Resistance: The body cannot use glucose efficiently.
- Hyperglycemia: Glucose accumulates in the bloodstream rather than entering cells.
- Complications: Persistent high blood sugar can lead to heart disease, kidney disease, nerve damage, and vision problems.
Weight loss is a medical necessity. Even losing a small percentage of body weight can reduce insulin resistance, lower blood pressure, improve cholesterol, and sometimes decrease the need for medication.
Step 1: Set Short-Term and Long-Term Goals
Effective weight management requires a strategic approach. Goals should be SMART: Specific, Measurable, Attainable, Relevant, and Time-bound.
-
Short-Term Goals: Build momentum and provide immediate motivation.
- Examples: “I will walk for 30 minutes daily this week” or “I will add one serving of vegetables to dinner for the next two weeks.”
-
Long-Term Goals: Keep you focused on the broader clinical objective.
- Examples: “I will lose 10 pounds in three months” or “I will reduce my A1C to a healthy range within six months.”
Flexibility is essential. Adjust goals as life changes, but maintain commitment to improving metabolic health.
Step 2: Master Portion Sizes
Portion control is key to weight loss and blood sugar management. Overeating can cause spikes in glucose levels, while under-eating can trigger hypoglycemia. The goal is moderation, not deprivation.
Strategies:
- Visualize Portions: A serving of pasta is typically half a cup—far less than restaurant portions.
-
The Plate Method: Divide your plate visually:
- 50% non-starchy vegetables
- 25% lean protein
- 25% grains or carbohydrate-rich foods
- Dishware Selection: Smaller plates and bowls can naturally reduce intake by altering visual perception.
Step 3: Implement Dietary Changes
A balanced diet helps manage weight and stabilize blood sugar. Focus on two things:
Increase Fruits and Vegetables
These foods are nutrient-dense, high in fiber, and generally low in calories. Fiber slows digestion, promotes satiety, and helps prevent glucose spikes.
- Eat the Rainbow: include a variety of colors to ensure a broad intake of vitamins, minerals, and antioxidants.
-
Add Vegetables to Every Meal: vegetable omelets for breakfast, raw veggies for snacks, and colorful vegetables on half your dinner plate.
Reduce Added Sugar and Processed Foods
Added sugars and processed foods often cause rapid glucose spikes, provide empty calories, and contain unhealthy fats.
- Read Labels: Avoid products where sugar or syrup appears among the first ingredients.
- Choose Whole Foods: Opt for whole grains, lean proteins, and low-fat dairy over pre-packaged alternatives.
Step 4: Incorporate Regular Physical Activity
Exercise is non-negotiable for enhancing insulin sensitivity. When you exercise, your cells become more responsive to insulin, improving glucose regulation.
Activity does not require a gym membership. So, walking, gardening, or taking the stairs all count. Small, consistent actions, like standing instead of sitting, cumulatively contribute to improved metabolic health.
Step 5: Aim for 150 Minutes of Exercise Weekly
The American Diabetes Association recommends 150 minutes of moderate-intensity exercise per week.
- Moderate Intensity: Activities that raise your heart rate and breathing but still allow conversation (e.g., brisk walking, cycling, water aerobics).
- Frequency: Spread exercise over at least three days, avoiding more than two consecutive inactive days.
- Progression: Start with 10-minute sessions if you’re sedentary and gradually increase duration.
Step 6: Monitor and Adjust
Monitoring provides insight into how your body responds to food, exercise, and stress.
- Tools: Use a glucose meter or Continuous Glucose Monitor (CGM).
- Pattern Recognition: Track spikes after high-carb meals or drops after exercise.
- Medication Adjustment: Weight loss may improve insulin sensitivity and reduce medication needs. Regular monitoring ensures safe adjustments.
Step 7: Maintain Commitment and Resilience
Weight management is a long-term process. Setbacks, like holidays or stressful weeks, are normal. Understand that a lapse in diet or exercise does not define failure. The critical factor is the ability to resume your regimen immediately.
Utilize weekly weigh-ins and glucose logs to stay accountable.
And mostly, acknowledge non-scale victories, such as resisting sugary foods or completing a workout week, to sustain motivation.
The Clinical Connection: Weight Loss and Glycemic Control
Successful weight loss directly improves blood sugar control. Reducing body fat decreases insulin resistance, allowing the body to use insulin more efficiently. For many, this can reduce medication dependence and improve overall well-being.
Conclusion
Following these steps supports lower blood glucose, reduced insulin resistance, and improved health.
To further support your weight loss efforts and diabetes management, specific supplementation can be integrated into your routine:
- Weight Loss Formula Keto Diet Energy Levels: Supports weight management and energy optimization for diabetics.
- Moringa Capsules: Helps with weight loss and blood sugar management.
- Maca Root: Supports hormonal balance and energy during weight loss.
The ultimate goal is not just a lower number on the scale. It’s a healthier, more fulfilling life.
Frequently Asked Questions
Why is it harder to lose weight with Type 2 diabetes?
Insulin resistance can make weight loss more challenging because the body struggles to efficiently process glucose for energy. Furthermore, certain diabetes medications can contribute to weight gain as a side effect.
What is the Plate Method for diabetic weight loss?
The Plate Method involves filling 50% of your plate with non-starchy vegetables. The remaining half is split equally between 25% lean protein and 25% complex carbohydrates to stabilize glucose levels.
Can I stop my medication if I lose significant weight?
Significant weight loss can sometimes lead to a reduction in medication or even diabetes remission. However, you must never stop or adjust your dosage without the direct supervision of your healthcare provider.
How does exercise specifically help with weight loss in diabetics?
Exercise allows your muscles to use glucose for energy without requiring as much insulin. This process lowers blood sugar levels and improves your metabolic health and insulin sensitivity over the long term.
Written By Dr. Ahmet Ergin
470 total articles
Meet Dr. Ahmet Ergin, a highly skilled and dedicated endocrinologist with a passion for diabetes care. Dr. Ergin earned his medical degree with honors from Marmara University in Istanbul. He completed internal medicine residency and endocrinology fellowship at Cleveland Clinic. Dr. Ergin is board-certified in Internal Medicine, Endocrinology, Diabetes, and Metabolism due to his vast medical expertise. He's a certified diabetes educator, author of “The Ultimate Diabetes Book,” and founder of “the SugarMD YouTube channel.” Dr. Ergin offers exceptional diabetes care to his patients in Port Saint Lucie, FL, helping them manage effectively. For a closer look into his insights and experiences, connect with Dr. Ahmet Ergin on LinkedIn, Instagram, and YouTube.”
Disclaimer: These statements have not been evaluated by the Food and Drug Administration. Information on this website isn't intended to treat, cure or prevent any disease. Discuss with your doctor and do not self-treat.
Products