Dexcom: How Often To Change Sensor


Table of Contents
- Summary
- What Is a Dexcom Sensor?
- Dexcom Sensors: How Often Do You Change Them?
- Standard Wear Time for Dexcom Sensors
- Dexcom G6 Sensor: How Long Does It Last?
- Dexcom G6 Wear Time
- Dexcom G6 Transmitter
- What Happens When the Session Ends
- Dexcom G7 Sensor: How Long Does It Last?
- Dexcom G7 Wear Time
- Dexcom G7 Grace Period
- Built-In Transmitter
- Dexcom ONE+: How Long Does It Last?
- Dexcom ONE+ Sensor Wear Time
- ONE+ Grace Period
- Can You Extend a Dexcom Sensor Past the Recommended Time?
- Dexcom Sensors Are Single-Use
- Why Extending Wear Time May Be Risky
- What If Your Dexcom Sensor Stops Working Early?
- Common Reasons a Sensor May Fail Early
- Dexcom Replacement Support
- Signs It’s Time to Replace Your Sensor (Even Before the End Date)
- Tips for Better Sensor Wear (So It Lasts the Full Session)
- Apply to Clean, Dry Skin
- Choose a Good Placement Site
- Areas to Avoid
- Use Extra Adhesive Support if Needed
- Rotate Sensor Sites
- What Happens to Accuracy Over the 10-Day Wear Period?
- Day 1: Adjustment Phase
- Days 2–7: Most Stable Period
- Days 8–10: Late Wear Performance
- Grace Period (G7 & ONE+)
- Dexcom Model Comparison Table
- Can You Insert a New Sensor Before the Old One Ends?
- Ending a Session Early
- Overlapping Warm-Up Timing
- Best Practice Strategy
- Quick Troubleshooting Checklist Before Replacing a Sensor
- Basic Connection Checks
- Model-Specific Checks (G6 Users)
- Signal or Reading Issues
- Adhesive and Site Inspection
- When to Confirm with a Fingerstick
- What Happens If You Don’t Change Your Dexcom On Time?
- How SugarMD Supports Your Dexcom Journey
- Conclusion
- Frequently Asked Questions
- How often do you change a Dexcom sensor?
- How long can I wear a Dexcom G6 sensor?
- Does Dexcom G7 have a grace period?
- Can I restart a Dexcom sensor after it ends?
- Why does my Dexcom fail on day 9 or 10?
- Can sweating cause Dexcom sensors to fall off?
- Can you shower or swim with a Dexcom?
- Can exercise affect Dexcom accuracy?
- What should I do if my Dexcom sensor fails early?
- Does insurance replace Dexcom sensors that fail early?
Summary
- Dexcom sensors are designed to be changed every 10 days for accurate glucose readings.
- Dexcom G7 and Dexcom ONE+ include a 12-hour grace period after the 10-day wear time.
- Dexcom G6 uses a separate transmitter that lasts about 90 days, while G7 has a built-in transmitter.
- Extending sensor wear beyond the recommended time can reduce accuracy and increase errors.
- Early sensor failure can occur due to adhesion issues, signal loss, or pressure during sleep.
Dexcom CGMs help people monitor glucose in real time without constant fingersticks. Their sensors are designed to be replaced every 10 days. Doing so on schedule helps maintain accuracy, comfort, and reliable glucose readings.
In this guide, we will break down sensor wear time for the Dexcom G6, G7, and Dexcom ONE+. We also cover grace periods, early failures, and common replacement tips.
What Is a Dexcom Sensor?
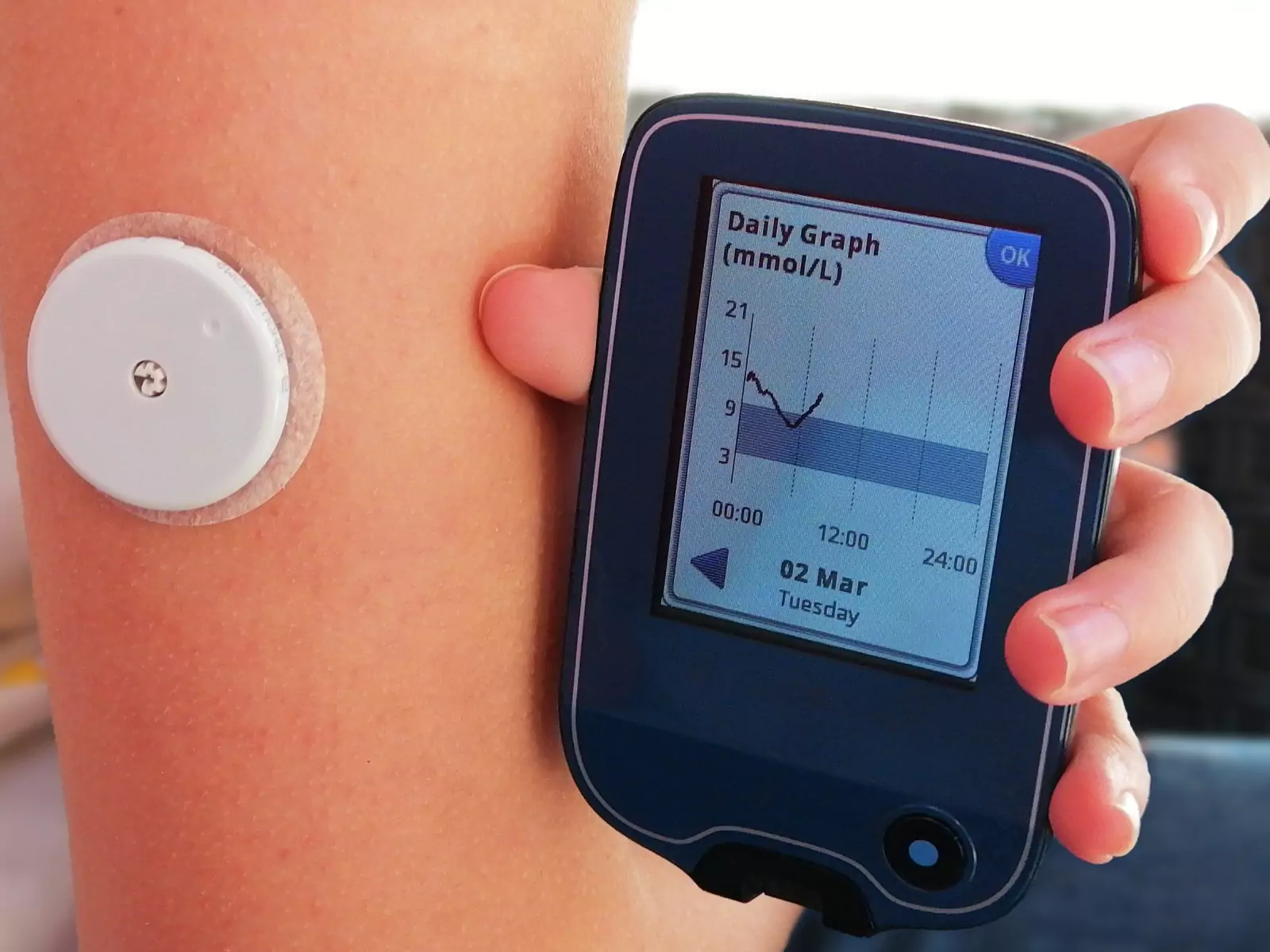
The Dexcom sensor is the wearable component of the continuous glucose monitoring system. It sits on your body and measures glucose levels through interstitial fluid just beneath the skin.
The sensor sends glucose readings to:
- A mobile app
- A dedicated receiver
- Other compatible devices, depending on the Dexcom model
Sensors track glucose continuously and must be replaced on schedule to maintain accuracy and reliability.
Dexcom Sensors: How Often Do You Change Them?
Standard Wear Time for Dexcom Sensors
All Dexcom sensors are designed to be worn for up to 10 days, including:
- Dexcom G6
- Dexcom G7
- Dexcom ONE+
Dexcom G6 Sensor: How Long Does It Last?
Dexcom G6 Wear Time
Dexcom G6 sensors are intended for up to 10 days of continuous use. The system will notify you as the session approaches its end.
Dexcom G6 Transmitter
The G6 uses a separate reusable transmitter that snaps into the sensor. This transmitter typically lasts around 90 days.
For a detailed breakdown of pricing and replacement timing, see our guide on Dexcom G6 cost.
What Happens When the Session Ends
Your Dexcom device alerts you when the session is ending. You must stop the current session before inserting and starting a new sensor.
Dexcom G7 Sensor: How Long Does It Last?
Dexcom G7 Wear Time
Dexcom G7 sensors are intended for 10 days of use.
Dexcom G7 Grace Period
Dexcom G7 includes a 12-hour grace period after the 10-day session, giving extra flexibility. Total possible wear time is about 10.5 days.
Built-In Transmitter
Unlike the G6, the G7 has the transmitter built into the sensor. When you replace the sensor, you automatically replace the transmitter. This simplifies setup and reduces the number of components you need to manage.
Dexcom ONE+: How Long Does It Last?
Dexcom ONE+ Sensor Wear Time
ONE+ sensors are designed for up to 10 days of continuous glucose monitoring.
ONE+ Grace Period
Like the G7, the Dexcom ONE+ includes a 12-hour grace period, helpful for traveling, working, or changing sensors later in the day.
Can You Extend a Dexcom Sensor Past the Recommended Time?
Dexcom Sensors Are Single-Use
Dexcom sensors are disposable and not designed to be restarted or extended.
Why Extending Wear Time May Be Risky
- Accuracy may decrease
- Sensor errors may increase
- Adhesive failure becomes more likely
- Skin irritation risk may rise
What If Your Dexcom Sensor Stops Working Early?
Common Reasons a Sensor May Fail Early
- Sensor error or signal loss
- Adhesive peeling or detaching
- Compression lows (pressure on the sensor during sleep)
- Bleeding or discomfort at the insertion site
Dexcom Replacement Support
If your sensor fails early, contact Dexcom support. Depending on the issue and your policy, they may provide a replacement.
Signs It’s Time to Replace Your Sensor (Even Before the End Date)
- Repeated sensor errors or “brief sensor issue” messages
- Frequent readings inconsistent with fingerstick or symptoms
- Adhesive pulling off or sensor lifting
- Increasing redness, itching, burning, or swelling
Tips for Better Sensor Wear (So It Lasts the Full Session)
Apply to Clean, Dry Skin
Avoid lotions, oils, and heavy moisturizers before placement. Ensure skin is fully dry.
Choose a Good Placement Site
Using the manufacturer-approved insertion sites ensures the algorithm processes your interstitial fluid correctly.
- Dexcom G6: Abdomen (for adults) and upper buttocks (for children 2–17 years old).
- Dexcom G7: Back of the upper arm (primary site for adults).
- Dexcom ONE+: Back of the upper arm.
Areas to Avoid
Adhesion peeling and inaccurate readings can occur if the sensor is placed in high-risk areas. Avoid:
- Scar tissue or stretch marks, where fluid flow may be altered.
- Within 2 inches of insulin injection or pump infusion sites.
- High-friction areas such as waistbands or tight clothing zones.
- Sleeping directly on the sensor, which can compress the interstitial fluid
Use Extra Adhesive Support if Needed
Excess moisture trapped under the adhesive can cause the patch to lift prematurely. Overpatches or medical tape can help prevent peeling, especially during:
- Sweating
- Swimming
- Workouts
- Hot climates
Rotate Sensor Sites
Avoid using the same spot repeatedly. This reduces irritation and improves comfort.
What Happens to Accuracy Over the 10-Day Wear Period?
Day 1: Adjustment Phase
Most early failures occur within the first 24 hours.
During this time:
- Interstitial fluid is adjusting around the inserted sensor
- Minor variability compared to fingerstick may occur
- Avoid aggressive treatment decisions unless readings match symptoms
Days 2–7: Most Stable Period
This is typically the most reliable portion of the wear cycle.
During this phase:
- Algorithm fully calibrated
- Trend analysis is reliable
- Users report the highest confidence in readings
Days 8–10: Late Wear Performance
Toward the end of the session, some users may notice subtle changes such as:
- Possible signal lag during rapid glucose swings
- Mild accuracy drift compared to fingerstick checks
- Increased brief sensor issue notifications in rare cases
Not all users experience late-wear variability, but confirming with a fingerstick may be appropriate if readings are inconsistent.
Grace Period (G7 & ONE+)
- System remains functional
- Not intended for extended medical decisions
- Dexcom limits official wear time for safety
Dexcom Model Comparison Table
|
Feature |
G6 |
G7 |
ONE+ |
|
Wear Time |
10 Days |
10 Days |
10 Days |
|
Grace Period |
No |
12 Hours |
12 Hours |
|
Warm-Up Time |
2 Hours |
30 Minutes |
30 Minutes |
|
Transmitter |
Separate (lasts 90 days) |
Built-In |
Built-In |
|
Sensor Size |
Larger |
Smaller |
Similar to G7 |
While wear duration is consistent across models, G7 and ONE+ improve convenience with shorter warm-ups and built-in transmitters. G6 remains widely integrated with automated insulin delivery systems, making it a strong option for pump users.
The Dexcom G6 also has automated insulin delivery systems, as its separate transmitter design integrates with many leading AID pumps.
Can You Insert a New Sensor Before the Old One Ends?
Ending a Session Early
If you choose to switch sensors before the full 10-day period:
- Manually stop the current session in the Dexcom app or receiver.
- Remove the existing sensor.
- Insert the new sensor and begin the warm-up period.
For G6 users, this will trigger a 2-hour warm-up. For G7 and ONE+, the warm-up lasts 30 minutes.
Overlapping Warm-Up Timing
Some users prefer to insert the new sensor shortly before ending the old one to reduce downtime. However, the system does not allow two active sensors at once. The old session must be stopped before the new warm-up begins.
To minimize interruption:
- Avoid switching during rapid glucose changes.
- Plan the transition when glucose levels are stable.
- Avoid making major insulin adjustments during the warm-up window.
Best Practice Strategy
For minimal data gaps, switch during stable glucose periods for minimal disruption.
- G6 users may prefer changing sensors in the evening when fewer dosing decisions are needed.
- G7 and ONE+ users have greater flexibility due to the shorter warm-up time.
- If using automated insulin delivery systems, confirm system pairing after inserting the new sensor.
Quick Troubleshooting Checklist Before Replacing a Sensor
Basic Connection Checks
- Confirm Bluetooth is enabled on your phone or receiver
- Make sure the Dexcom app is open and running properly
- Restart the app if readings stop updating
- Keep your device within range of the transmitter
Model-Specific Checks (G6 Users)
- Confirm the transmitter is fully snapped into the sensor
- Inspect the transmitter for visible damage
- Verify the transmitter battery has not expired
Signal or Reading Issues
- Wait 15–20 minutes after signal loss
- Review any error messages
- Avoid lying directly on the sensor to rule out compression lows
- Compare readings with symptoms before assuming failure
Adhesive and Site Inspection
- Check if the adhesive is lifting or peeling
- Look for redness, swelling, or irritation
- Ensure the sensor has not shifted from its insertion angle
Troubleshooting first can prevent unnecessary replacements and reduce sensor waste.
When to Confirm with a Fingerstick
Situations to check with a fingerstick:
- Rapid glucose changes
- Symptoms don’t match readings
- End-of-wear period
- Sensor error alerts
What Happens If You Don’t Change Your Dexcom On Time?
-
Accuracy Risks:
- lag during rapid glucose changes
- sensor drift, where readings gradually differ from true glucose values
- calibration mismatch
-
Skin Health Concerns:
- irritation
- local inflammation
- adhesive breakdown
- higher risk of minor infection in sensitive individuals
- System Shutdown: automatic session ending, grace period expiration, restarts are unreliable
How SugarMD Supports Your Dexcom Journey
SugarMD helps patients across the country get access to Dexcom through:
- Prescription and insurance paperwork support
- Appeals and follow-ups for denied claims
- Telemedicine & remote glucose monitoring through SugarMD
If you’re ready to simplify your diabetes care and want help with the Dexcom process, the team at SugarMD can guide you every step of the way.
Conclusion
Most Dexcom sensors are designed to change every 10 days. The Dexcom G7 and ONE+ models include a 12-hour grace period for easier replacement.
Replacing sensors on schedule helps improve accuracy, comfort, and reliability. If your sensor fails early, check the troubleshooting steps and contact support for a replacement.
Frequently Asked Questions
How often do you change a Dexcom sensor?
Every 10 days. The G7 and ONE+ models offer an additional 12-hour grace period for more flexibility.
How long can I wear a Dexcom G6 sensor?
Up to 10 days, with the separate transmitter lasting ~90 days.
Does Dexcom G7 have a grace period?
Yes. The G7 includes a 12-hour grace period after the 10-day session ends.
Can I restart a Dexcom sensor after it ends?
No, restarting is not recommended. Attempting to extend wear time can result in inaccurate readings and safety issues.
Why does my Dexcom fail on day 9 or 10?
Late-wear failures typically happen because the sensor's internal chemical coating has naturally degraded, or the medical adhesive has simply worn out from days of friction and moisture.
Can sweating cause Dexcom sensors to fall off?
Yes, trapped moisture can weaken adhesive. Use an overpatch if needed.
Can you shower or swim with a Dexcom?
Yes, Dexcom sensors are water-resistant and safe for showering and swimming. However, frequent exposure to water can degrade the adhesive faster, making an overpatch highly recommended.
Can exercise affect Dexcom accuracy?
Yes. Rapid glucose changes or hydration shifts can cause temporary sensor lag.
What should I do if my Dexcom sensor fails early?
Check placement, adhesive, and signal first. Compare with a fingerstick. If it still fails, contact Dexcom support for a possible replacement.
Does insurance replace Dexcom sensors that fail early?
Insurance may cover early replacements for defective sensors. Coverage varies by plan, so confirm with Dexcom or your provider.
Written By Dr. Ahmet Ergin
469 total articles
Meet Dr. Ahmet Ergin, a highly skilled and dedicated endocrinologist with a passion for diabetes care. Dr. Ergin earned his medical degree with honors from Marmara University in Istanbul. He completed internal medicine residency and endocrinology fellowship at Cleveland Clinic. Dr. Ergin is board-certified in Internal Medicine, Endocrinology, Diabetes, and Metabolism due to his vast medical expertise. He's a certified diabetes educator, author of “The Ultimate Diabetes Book,” and founder of “the SugarMD YouTube channel.” Dr. Ergin offers exceptional diabetes care to his patients in Port Saint Lucie, FL, helping them manage effectively. For a closer look into his insights and experiences, connect with Dr. Ahmet Ergin on LinkedIn, Instagram, and YouTube.”
Disclaimer: These statements have not been evaluated by the Food and Drug Administration. Information on this website isn't intended to treat, cure or prevent any disease. Discuss with your doctor and do not self-treat.
Products