Summary:
- Hyperlipidemia refers to elevated levels of cholesterol and triglycerides in the blood.
- It often causes no symptoms, which is why many people don’t know they have it.
- A lipid panel blood test is the primary way to diagnose the condition.
- Treatment focuses on lifestyle changes and medications based on overall cardiovascular risk.
What is Hyperlipidemia? A Complete Guide
Hyperlipidemia is the medical term for high levels of lipids (fats) in the blood. These lipids mainly include cholesterol and triglycerides. While the body needs them in small amounts, elevated levels can quietly increase the risk of serious health problems.
One of the challenges with hyperlipidemia is that it does not usually cause noticeable symptoms. Many people only discover it during routine blood work. According to the Centers for Disease Control and Prevention, about 86 million adults aged 20 or older have total cholesterol levels above 200 mg/dL, often without realizing it.
Over time, untreated hyperlipidemia can lead to heart disease, stroke, and other complications. It is also commonly seen alongside conditions like fatty liver disease and diabetes due to shared metabolic factors.
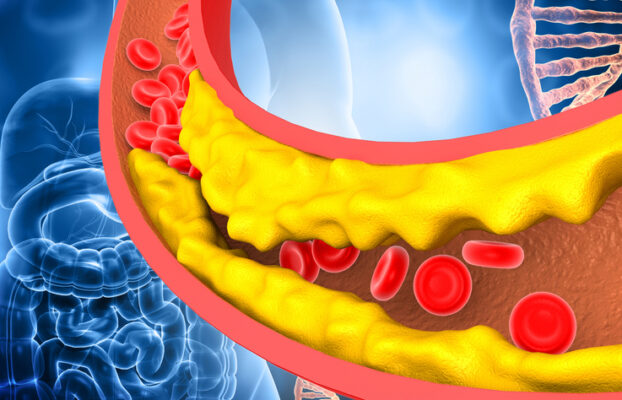
Hyperlipidemia Defined
Hyperlipidemia simply means high levels of fats in the bloodstream. These fats include cholesterol and triglycerides.
The term is often used interchangeably with:
- high cholesterol
- dyslipidemia
However, hyperlipidemia is broader because it includes both cholesterol and triglyceride abnormalities.
What Lipids are Included in a Lipid Panel?
A lipid panel measures different types of fats in the blood. Understanding each one helps clarify how risk is assessed.
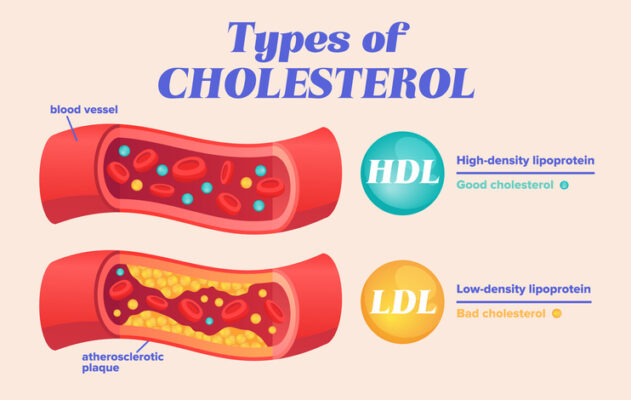
LDL (Bad Cholesterol)
Low-density lipoprotein contributes to plaque buildup inside arteries. Higher levels increase the risk of heart attack and stroke.
HDL (Good Cholesterol)
High-density lipoprotein helps remove excess cholesterol from the bloodstream. Higher levels are generally protective.
Triglycerides
Triglycerides are a form of stored fat used for energy. Elevated levels increase cardiovascular risk, and very high levels may increase the risk of pancreatitis.
Total Cholesterol
This is an overall measure that includes LDL, HDL, and a portion of your triglyceride levels. Total cholesterol under 200 mg/dL is generally considered healthy for most adults.
Why is Hyperlipidemia Dangerous?
Hyperlipidemia is dangerous because excess lipids circulate silently and damage blood vessels over time.
Atherosclerosis and Plaque Formation
When LDL cholesterol and other lipids remain elevated, they can deposit inside artery walls. This process, known as atherosclerosis, leads to plaque buildup that makes arteries:
- Narrower
- Less flexible
- More likely to become blocked
Reduced blood flow limits oxygen delivery to vital organs and increases the risk of sudden cardiovascular events.
Health Risks Linked to Untreated High Lipids
If not managed, hyperlipidemia can lead to:
- Coronary artery disease
- Heart attack
- Stroke
- Peripheral artery disease
These complications often develop silently over many years.
Does Hyperlipidemia Cause Symptoms?
Hyperlipidemia is usually a silent condition. Most people feel well until serious complications develop.
When Symptoms May Appear
Symptoms typically appear only after blood flow becomes restricted. These may include:
- chest pain during activity
- shortness of breath
- leg pain during walking
- stroke-like symptoms such as sudden weakness or trouble speaking
Clinical guidance from the American Heart Association explains that these symptoms reflect cardiovascular disease caused by long-standing plaque buildup rather than high cholesterol itself.
Rare Visible Signs
In rare cases, particularly with genetic lipid disorders, physical signs may appear, including:
- xanthomas, fatty deposits under the skin or along tendons
- corneal arcus, a gray or white ring around the iris
Because symptoms usually appear late, routine blood testing is essential for early detection and prevention of cardiovascular complications.
Common Causes and Risk Factors
Hyperlipidemia usually develops from a combination of lifestyle, medical, and genetic factors.
Lifestyle-Related Factors
- diets high in saturated and trans fats
- lack of physical activity
- overweight or obesity
- smoking
- excess alcohol intake
These are among the most common contributors.
Medical Conditions
Certain conditions can increase lipid levels, including:
- diabetes and insulin resistance
- hypothyroidism
- chronic kidney disease
- some liver conditions
Genetic Causes
Some people inherit conditions such as familial hyperlipidemia. These cases often involve very high cholesterol levels at a younger age and may require early treatment.
How Hyperlipidemia is Diagnosed
Lipid Panel Blood Test
A lipid panel is the primary blood test used to diagnose hyperlipidemia. This test measures the concentration of total cholesterol, LDL, HDL, and triglycerides in milligrams per deciliter (mg/dL).
Your healthcare provider may ask you to fast for 9 to 12 hours before the blood draw. However, non-fasting lipid profile screening is increasingly used for initial cardiovascular risk assessment.
Why Regular Screening Matters
Because high lipid levels are typically asymptomatic, regular screening is the only way to detect the condition early. Early detection allows for clinical interventions that can prevent long-term arterial damage.
According to the AHA guidelines for cholesterol testing, most healthy adults aged 20 or older should have their levels checked every 4 to 6 years. Those with existing risk factors, such as diabetes, may require more frequent monitoring.
Hyperlipidemia Treatment Options
Lifestyle changes
Lifestyle modification is the foundation of lipid management and may be sufficient for mild-to-moderate cases. Adopting consistent heart-healthy lifestyle habits can significantly improve cholesterol levels and reduce long-term cardiovascular risk.
Key strategies include:
- Heart-healthy eating patterns that reduce saturated and trans fats
- Regular physical activity
- Weight management
- Smoking cessation
- Limiting alcohol intake
Medications
Medication is recommended when lifestyle measures alone do not adequately reduce risk.
Common medication classes include:
- Statins, which lower LDL cholesterol and reduce the risk of heart attack and stroke
- Ezetimibe, which limits cholesterol absorption in the intestine
- Fibrates, often used when triglycerides are elevated
- PCSK9 inhibitors, injectable therapies for high-risk or inherited cases
- Omega-3 fatty acids, used selectively for high triglycerides
Treatment Depends on Overall Risk
Treatment decisions are based on several factors, including:
- age
- diabetes status
- blood pressure
- smoking history
- prior heart disease
This is why two people with similar cholesterol levels may receive different treatment plans.
Hyperlipidemia and Diabetes
There is a strong connection between hyperlipidemia and diabetes.
Why Diabetes Increases Risk
People with diabetes face a significantly higher risk of heart disease. The relationship between hyperlipidemia and diabetes is well established, as high blood sugar and insulin resistance worsen lipid abnormalities and accelerate artery damage.
Diabetic Dyslipidemia Pattern
This pattern often includes:
- Elevated triglycerides
- Low HDL
- LDL particles that are more atherogenic
Why Cholesterol Control Matters in Diabetes
Managing lipids helps reduce long-term complications and is a core part of diabetes care alongside glucose and blood pressure management.
Foods to Limit and Foods to Focus On
Diet plays a major role in managing lipid levels. Making the right choices can support long-term heart health.
Foods to Limit
Certain foods can worsen cholesterol and triglyceride levels when consumed frequently.
- fried and highly processed foods
- trans fats
- high saturated fat sources
- sugary drinks and refined carbohydrates
These can contribute to both elevated LDL and triglycerides.
Foods to Focus On
Other foods can help support healthier lipid levels when included regularly.
- fiber-rich foods such as vegetables, legumes, and oats
- healthy fats like olive oil, nuts, and seeds
- lean protein sources
- fatty fish when appropriate
These choices can support better metabolic and cardiovascular health.
Frequently Asked Questions
Is Hyperlipidemia the Same as High Cholesterol?
Hyperlipidemia is a broader term that includes both high cholesterol and high triglycerides.
What Causes Hyperlipidemia?
It can result from lifestyle factors, medical conditions, or inherited genetic disorders.
Can You Have Hyperlipidemia With No Symptoms?
Yes, most people do not experience symptoms until complications develop.
What’s the Difference Between LDL and HDL?
LDL contributes to plaque buildup, while HDL helps remove excess cholesterol.
What Triglyceride Level Is Considered High?
Levels above 150 mg/dL are considered elevated, while levels above 200 mg/dL are high.
How is Hyperlipidemia Treated?
Treatment typically includes lifestyle changes and, when needed, medications based on overall risk.
Conclusion
Hyperlipidemia refers to elevated levels of cholesterol and triglycerides that can quietly increase the risk of heart disease and stroke. Because it often develops without symptoms, regular screening plays a critical role in early detection.
Managing hyperlipidemia involves more than just lowering numbers. It requires a combination of lifestyle changes, proper nutrition, and medical guidance based on individual risk factors. With the right approach, it is a highly manageable condition that can significantly reduce long-term health risks.
Disclaimer: Any information on diseases and treatments on this website is for general guidance only and must never be a substitute for the advice your doctor or other qualified healthcare professional provides. Always seek the advice of your physician or other qualified health care professional with questions you may have regarding your medical condition.
